Research on T-cell therapy, which introduce CAR genes and T-cell receptors, is progressing as a treatment for both cancer and infectious disease. These treatments are difficult to develop, however, as autologous transplantation (harvest and reintroduction of blood stem cells) has a steep time and resource cost.
As a result of this, attention has been focused on allogeneic transplantation, where T-cells are generated from the cells of another person and transplanted into the patient. However, controlling the immune response to these foreign cells is a problem. Through the editing of iPS cell genomes and differentiation into T-cells, a research group including Bo Wang, researcher, and Professor Shin Kaneko of the Center for iPS Cell Research and Application, Kyoto University, succeeded in generating 'stealth fighter' T-cells that attack cancer cells without being generating an immune response. "We used T-cells in this study but using other differentiated cells may lead to other new therapies," Dr. Kaneko said. The results have been published in Nature Biomedical Engineering.
Three major mechanisms for eliminating foreign T-cells are known. These are: CD8T cells (which recognize HLA-I), CD4T cells (which recognize HLA-II), and NK-cells (Natural Killer cells- a type of lymphocyte). The research group introduced four genetic modifications at the iPS cell stage to suppress these immune responses. Specifically, after eliminating the HLA class 1 molecule, the HLA class 2 molecule was eliminated and two ligands involved in the activity of NK cells were modified. Previous studies have found that NK cells recognize other cells through various receptor groups and confirmed that there are NK cells that cannot be controlled by HLA-E alone.
In this study, researchers found that the ligand PVR was strongly related to the regulation of NK-cells and, after the introduction of HLA-E to the T-cell, activity of this ligand was knocked-out. The iPS cell-derived T-cells that had undergone these four genetic modifications were mixed with the peripheral blood of another person and the reaction was observed. The greater the number of genetic modifications, the weaker the immune response. In particular, the avoidance rate from NK cells was improved compared with that for the conventional method. Additionally, immunocompromised mice transplanted with human immune cells were transplanted with B-lymphoproliferative tumors and three T-cells every 9 days to determine tumor changes. The results showed that the increase in tumor cells was suppressed immediately after transplantation in the group transplanted with genome-edited T-cells compared with that the group transplanted with non-genome-edited iPS cell-derived T-cells (CAR gene transfer). In addition, the tumor was controlled after multiple transplantations.
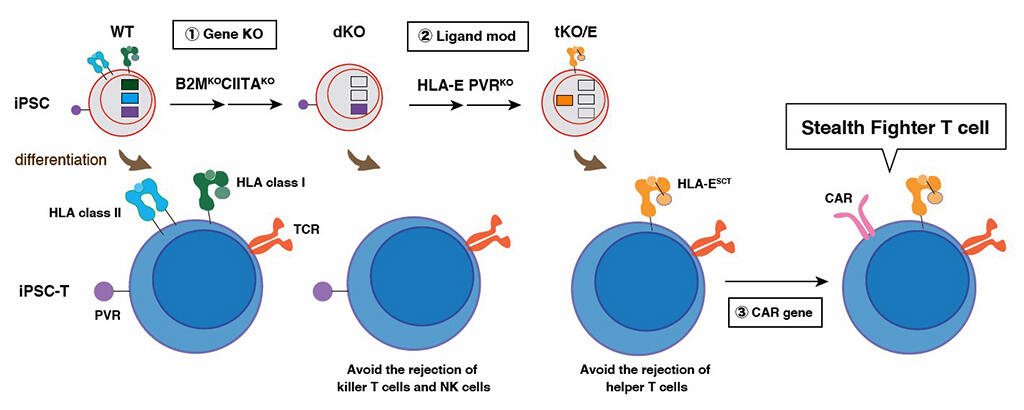
Source: Shin Kaneko Research Team of the Center for iPS Cell Research and Application (CiRA), Kyoto University
To date, various studies have been conducted to perform genome editing directly on T-cells; however, performing genome editing has always weakened the potency of T-cells. By undertaking genome editing while T-cells are still iPS cells and then differentiating them, the researchers succeeded in producing stealth fighter T-cells. These cells prevent the weakening of T-cells and are not attacked by the immune cells of the recipient.
This article has been translated by JST with permission from The Science News Ltd.(https://sci-news.co.jp/). Unauthorized reproduction of the article and photographs is prohibited.




