The research group of Associate Professor Kentaro Mizuno and others in the Department of Pediatric Urology, Graduate School of Medicine, Nagoya City University, has succeeded in discovering a new index for predicting future fertility in patients with cryptorchidism (a congenital disease in which the testis does not descend into the scrotum via the normal development path). Cryptorchidism is a highly variable disease, with differences in pretreatment testicular location, testicular size, mobility, and complications. Moreover, the age at the time of diagnosis and surgery also varied, and the normal range of serum hormone (inhibin B, AMH) levels differed depending on the age at which they were collected. There was even some debate among the co-authors on the best interpretation of the results. The study group proceeded to determine whether serum hormone levels could predict impaired spermatogenesis in cryptorchidism.
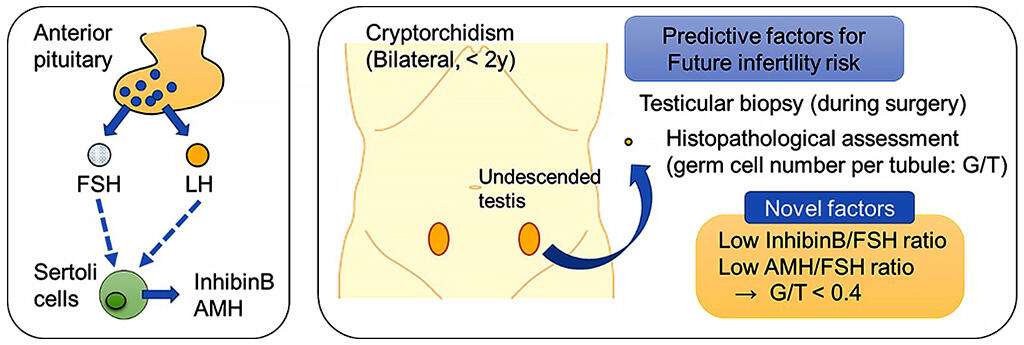
Kato T, Mizuno K, Nishio H, Hayashi Y, et al. J Urol. 207: 701-9, 2022
Provided by Nagoya City University
From this background, the authors studied 323 children with cryptorchidism who underwent surgery at Nagoya City University Hospital between December 2014 and May 2019, examining the age at surgery, affected side, pretreatment testicular location, pretreatment serum hormone levels (FSH, LH, testosterone, AMH, inhibin B), testicular size (volume), and testicular tissue findings. Statistical analysis was then carried out in 145 cases, excluding cases complicated with other diseases and data deficiency, etc. In cases with cryptorchidism (unilateral or bilateral), the serum inhibin B level was significantly lower in the bilateral cases than in the unilateral cases, and the G/T level (germ cells per tubule) was significantly decreased as well. Neither unilateral nor bilateral changes in hormone levels nor G/T were observed when the location of cryptorchidism before treatment (intraperitoneal, intrainguinal, or suprascrotal) changed.
Further, since serum hormone levels are known to vary greatly between 1 and 2 years after birth, the authors conducted an analysis restricted to individuals aged 2 years or younger. In the bilateral cases under 2 years old, the serum inhibin B/FSH ratio was significantly lower than that in the unilateral cases, and the G/T was also significantly lowered. In addition, the serum inhibin B/FSH ratio and AMH/FSH ratio were positively correlated with G/T. Since cases with a G/T of 0.4 or less on testicular biopsy are more likely to experience future spermatogenic impairment and are considered a high-risk group for male infertility, they performed ROC analysis when a G/T of 0.4 or less was correlated according to serum hormone levels. These results suggest that a lower inhibin B/FSH ratio or AMH/FSH ratio and a higher FSH value may predict a G/T of 0.4 or less.
"Based on the results we obtained, we wish to determine if similar results can be obtained in other populations," Associate Professor Mizuno said. "We aim to enable future fertility risk assessment before cryptorchidism surgery. Cryptorchidism is often observed in early childhood; as such, attention can be paid to surgical treatment at that time, but for children, the growth and sexual maturation process is of paramount importance. If we can determine the effects of sex hormones on the cellular differentiation and maturation mechanisms of testicular tissue, this will lead to therapeutic applications for male infertility."
This article has been translated by JST with permission from The Science News Ltd.(https://sci-news.co.jp/). Unauthorized reproduction of the article and photographs is prohibited.




