Type 2 innate lymphoid cells play a key role in inducing inflammation and aggravating allergic diseases such as asthma and atopic dermatitis, so researchers hope to develop new treatment methods that suppress the proliferation/function of these cells. A research group consisting of Professor Yasuo Shimizu of the Department of Pulmonary Medicine and Clinical Immunology, Dokkyo Medical University, Associate Professor Chie Sugimoto and Professor Hiroshi Wakao of the Host Defense Division, Research Center for Advanced Medical Science, Dokkyo Medical University and their colleagues has discovered that mucosal associated invariant T (MAIT) cells, which are natural immune-system T-cells, suppress asthma airway inflammation.
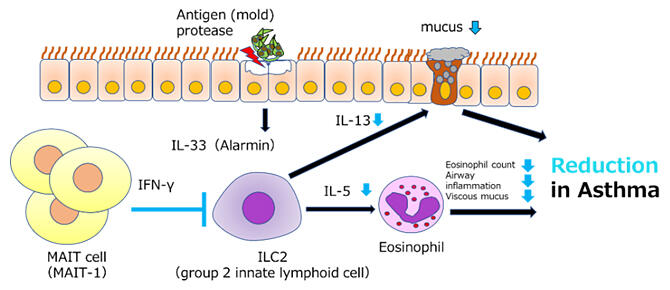
Provided by Dokkyo Medical University
MAIT cells are the largest cell group among human T-cells, but they only exist in tiny amounts in mice, which made it difficult to analyze pathological conditions. The research group used induced iPS cells from MAIT cells to develop a new mouse rich in MAIT cells and analyzed the pathology of asthma, thus clarifying that MAIT cells control asthma by repressing the proliferation of ILC2 (type 2 innate lymphoid cells), which cause airway inflammation, and repressing type 2 cytokine production.
To establish a mouse rich in MAIT cells, the group created and used iPS cells from mouse MAIT cells (MAIT-iPS cells). In wild-type mouse lungs, around 3% of the total T-cells are MAIT cells, but in the manufactured mouse rich in MAIT cells (the Vα19 mouse) the proportion was increased to around 40%.
From this, the group determined the quantities of infiltrated cells and inflammatory substances (cytokines) using a bronchoalveolar lavage, which serves as an indicator of asthma, to assess the effect of increasing MAIT cells on airway inflammation. Their results showed that eosinophils and ILC2 quantity was reduced in the Vα19 mouse when compared to the wild-type mouse. In addition to cytokines that encourage ILC2 proliferation, they were able to observe a reduction in the substances that work to aggravate airway inflammation in the Vα19 mouse. Furthermore, they saw a reduction in stained areas (reduced inflammation) in the Vα19 mouse when compared to the wild-type mouse when they carried out mucus staining to indicate the extent of the exacerbation of airway inflammation.
The source of this reduction was MAIT cells repressing the proliferation and function of ILC2, which play a key role in inducing and aggravating asthma. ILC2 also play a role in the exacerbation of illnesses other than allergic diseases, including autoimmune disorders and lifestyle diseases, so researchers hope that these MAIT cells that repress ILC2 proliferation and function will become major targets for drug discovery, leading to the development of clinical application in the future.
Shimizu commented on the result, 'Based on these outcomes, in the future we hope to regulate MAIT cell control functions for ILC2 and develop regenerative medicine using MAIT cells created from iPS cells, which will open the way for further treatment methods for asthma and allergies as well as treatment methods for illnesses associated with ILC2.'
Journal Information
Publication: Frontiers in Immunology
Title: Mucosal-associated invariant T cells repress group 2 innate lymphoid cells in Alternaria alternata-induced model of allergic airway inflammation
DOI: 10.3389/fimmu.2022.1005226
This article has been translated by JST with permission from The Science News Ltd. (https://sci-news.co.jp/). Unauthorized reproduction of the article and photographs is prohibited.




