A research group led by Special Researcher Yumi Kuninaka, Associate Professor Yuko Ishida and Professor Toshikazu Kondo of the Department of Forensic Medicine, Wakayama Medical University, announced that they have found that macrophage balance is important in the process of normal wound healing. The researchers found M1 and M2 macrophages to be differentially expressed during each of the early to late stages of the healing process, and this imbalance may be responsible for chronic wounds. The results are expected to lead to the development of treatments for chronic wounds that are difficult to treat and was published in Scientific Reports.
Provided by Wakayama Medical University
Skin wounds heal through a 4-step process of the homeostasis, inflammation, proliferation, and remodeling phases. Acute wounds are traumatic injuries and burns that heal in five to 14 days, whereas chronic wounds are those that do not heal over a period of time despite appropriate treatment. Bed sores and diabetic foot ulcers are typical examples of chronic wounds, while acute wounds are thought to transition to chronic wounds due to infection or deterioration of nutritional and general conditions.
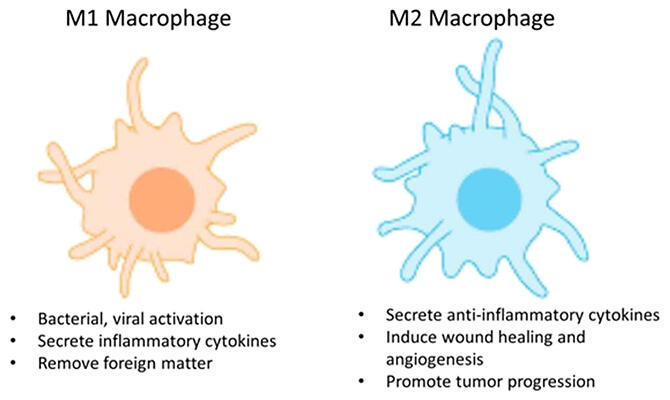
Macrophages are a type of white blood cell that is particularly active in trauma and acts as a cleaner, attacking and digesting pathogens and foreign substances in the body. Recent studies have reported that macrophages can be broadly divided into M1 and M2 macrophages, which can be polarized by extracellular stimuli and perform different functions depending on the situation. M1 macrophages are generally involved in pathogen and parasite defense while M2 are involved in tissue repair. Until now, the regulation of these macrophages, which have different functions in the wound healing process, was thought to be important for normal wound healing, but the details were a mystery.
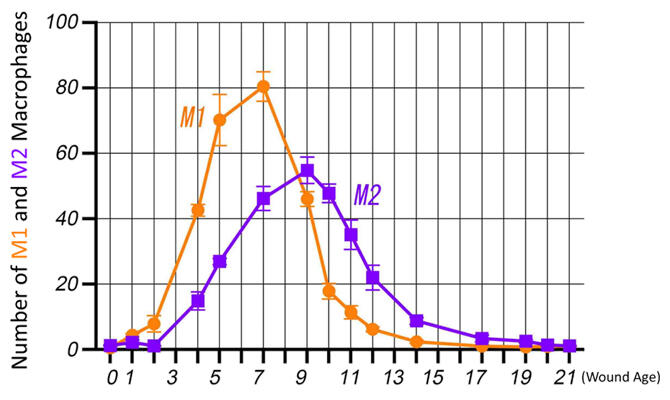
In the present study, the research group investigated the dynamics of these macrophages during the skin healing process in a mouse wound model using M1 and M2 polarisation markers. After doing so, they learned that the expression of M1 genes is then enhanced early in the healing process and M2 genes late in the healing process. Each had a different peak in expression. The researchers further analyzed these dynamics in human samples. They collected forensic autopsy human samples with known time since injury and consent to examine the dynamics of M1 and M2 macrophages several days after injury.
They found that, as in mice, M1 and M2 macrophages were activated early and late, respectively, resulting in successful healing. They also learned that if macrophages could be analyzed from the state of the wound and controlled appropriately, wounds could potentially be treated earlier and with minimal scarring while retaining their original morphology. In addition, forensic examination of the M1 macrophage/M2 macrophage ratio showed that the same value of 3.0 or more could be used as an indicator of within five days of injury.
Provided by Wakayama Medical University
"Macrophage imbalance is also thought to be involved in bedsores and diabetic foot ulcers," explained Ishida. "If we can understand the role of the balance of skin macrophages in the pathogenesis of various skin diseases as well as wounds, we can apply this to treatment. We hope to continue to contribute to the development of medicine through macrophages."
Journal Information
Publication: Scientific Reports
Title: Macrophage polarity and wound age determination
DOI: 10.1038/s41598-022-24577-9
This article has been translated by JST with permission from The Science News Ltd. (https://sci-news.co.jp/). Unauthorized reproduction of the article and photographs is prohibited.




