A research group led by Program-Specific Assistant Professor Norihide Jo and Professor Yoko Hamazaki of the Department of Life Science Frontiers, Center for iPS Cell Research and Application (CiRA), Kyoto University, in collaboration with Kyoto University Hospital, has conducted a detailed analysis of immune responses following vaccination with a COVID-19 vaccine and found that the slow onset of helper T-cell responses in the elderly is associated with a lower rate of antibody production and killer T-cell activation, and a lower frequency of adverse reactions. The study also found that antibody titers and immune responsiveness tended to be higher in people with systemic adverse reactions, such as fever, to the COVID-19 vaccine. The group's research was published in Nature Aging.
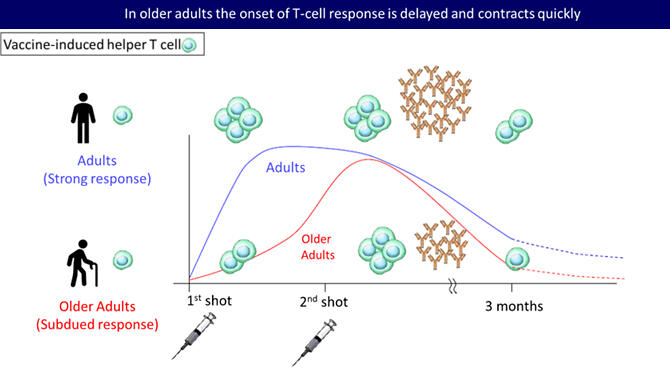
Provided by the Center for iPS Cell Research and Application, Kyoto University
Immune functions decline with age. This is because the thymus, the organ that produces T-cells, shrinks after puberty and the number of T-cells decreases, but this is balanced by an increase in immune memory to compensate. On the other hand, there are large individual differences in immune functions, even within the same age group. However, it is not well understood how and to what extent aging impacts the responsiveness of T-cells, which play a central role in immune responses against viruses and cancer, to stimulation in vivo. "Vaccination against COVID-19 is a rare opportunity for humans to receive a uniform antigenic stimulus," explained Hamazaki. "So that's why we undertook this study to understand the immune response."
A total of 216 people, approximately 100 elderly adults (aged 65 years and over) and adults (aged under 65 years), who had been vaccinated against COVID-19 with the Pfizer vaccine, volunteered for a study of T-cell responses following vaccination and how they were associated with antibody production and adverse reactions.
The researchers found that the helper T-cell response after vaccination in the elderly was characterized by a slow onset of the helper T-cell response and conversely a rapid contraction. Vaccine-specific helper T-cells in the elderly also expressed higher levels of PD1, a protein that suppresses T-cell activation, suggesting that the response was more likely to be subdued. "T-cell responses were 25-50% lower in the elderly, while PD1 was slightly less than two-fold higher in the elderly," commented Jo.
Regardless of age, they also found that individuals with a slower onset of the helper T-cell response had lower maximum antibody titers and killer T-cell activation, but were also less likely to experience systemic adverse reactions. According to Hamazaki, "We found that those who had a fever of 38℃ or higher had higher T-cell responses after the first vaccination and higher antibody titers after the second vaccination. We think that the high level of immune responsiveness results in the production of high levels of cytokines such as interferon-gamma, which causes fever." This would indicate that the key to improving vaccine efficacy is to enhance the helper T-cell response by initial vaccination and to ensure adequate cytokine production. Furthermore, it is clear that there are extremely large individual differences, as well as age differences, in these immune responses induced by vaccines. "Immune responses varied greatly between individuals, even in the same age group, with a 100-fold difference in the number of T-cells and cytokines between those with the highest and lowest levels," added Hamazaki.
The results of the study may be useful for the development of highly effective vaccines for the elderly and others whose immune functions are declining, and for the creation of vaccination schedules suited to the immune status of individuals. The research group is continuing to monitor the volunteers and will analyze the results to shed light on the mechanisms of age and individual differences in immune response. Moving forward, they hope that the scientific definition of immunity and immune aging will also help in the development of immune rejuvenation methods through immune aging interventions.
Journal Information
Publication: Nature Aging
Title: Impaired CD4+ T-cell response in older adults is associated with reduced immunogenicity and reactogenicity of mRNA COVID-19 vaccination
DOI: 10.1038/s43587-022-00343-4
This article has been translated by JST with permission from The Science News Ltd. (https://sci-news.co.jp/). Unauthorized reproduction of the article and photographs is prohibited.




